Welcome to Dr.Kathuria’s Dentistry 


-
 USA No
+18889812145
USA No
+18889812145
-
 UK No
+441970450032
UK No
+441970450032
-
 Australia No
+61384004931
Australia No
+61384004931
-
 Canada No
+18889812145
Canada No
+18889812145
-
 India Toll Free No
1800-11-7272
India Toll Free No
1800-11-7272



 USA No
+18889812145
USA No
+18889812145
 UK No
+441970450032
UK No
+441970450032
 Australia No
+61384004931
Australia No
+61384004931
 Canada No
+18889812145
Canada No
+18889812145
 India Toll Free No
1800-11-7272
India Toll Free No
1800-11-7272
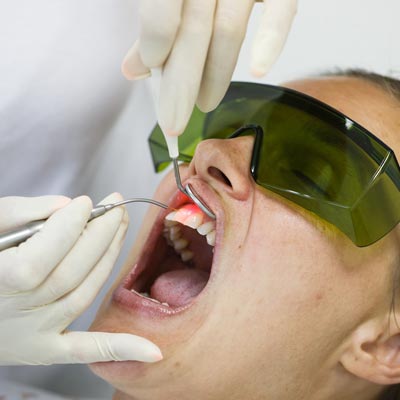
Gum disease refers to inflammation of the soft tissue (gingiva) and abnormal loss of bone that surrounds the teeth and holds them in place. Gum disease is the second most common cause of toothache.
Gum disease is caused by toxins secreted by bacteria in “plaque” that accumulate over time along the gum line. This plaque is a mixture of food, saliva, and bacteria.
Early symptoms of gum disease include gum bleeding without pain. Pain is a symptom of more advanced gum disease as the loss of bone around the teeth leads to the formation of gum pockets. Bacteria in these pockets cause gum infection, swelling, pain, and further bone destruction. Advanced gum disease can cause loss of otherwise healthy teeth.
Treatment of early gum disease involves oral hygiene and removal of bacterial plaque. Moderate to advanced gum disease usually requires a thorough cleaning of the teeth and teeth roots called “root planing” and “subgingival curettage.” Root planing is the removal of plaque and tartar (hardened plaque) from exposed teeth roots while subgingival curettage refers to the removal of the surface of the inflamed layer of gum tissue. Both of these procedures are usually performed under local anesthesia and may be accompanied by the use of oral antibiotics to overcome gum infection or abscess. Follow-up gum treatment may include various types of gum surgeries. In advanced gum disease with significant bone destruction and loosening of teeth, teeth splinting or teeth extractions may be necessary.
It is a progressive inflammatory disease of the gums and the surrounding tissue around the teeth. It is commonly known as gum disease and was referred to as pyorrhea in the old days. It is estimated that up to 80% of the population above the age of 40 may suffer from this disease with the severity varying drastically from one person to another. Periodontitis is the number one cause of tooth loss after the age of 40.
Certain medical conditions or medications can make you more susceptible to gum disease. They include pregnancy, diabetes, epilepsy, and such medications as chemotherapy, birth control pills, antidepressants, and those for heart problems.
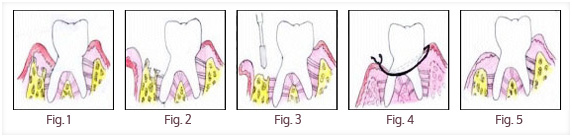
When gum is inflamed severely (periodontitis), alveolar bone will be absorbed, and defected. Periodontal ligaments which connect between the alveolar bone and the teeth will disappear. Sever bone lose will cause tooth moving and missing. Flap and bone surgery is order to contour the bone, deeply clean the tooth to reduce the inflammation, and promote bone re-growing and connections firm.
![]() SHONA
SHONA
Very much impressed with the amazing qualifications of both the doctors! The respect and care given was wonderful. The doctors and staff are very lovely people to deal with. “Many many thanks to Dr.Kathurias for my new smile and strong teeth.
![]() SABINE MONTAGNON
SABINE MONTAGNON
Everything went smooth and quickly doctors work well around my short schedule. Thank you Dr. Sween Kathuria for my new smile.
USA ![]()
Australia ![]()
Canada ![]()